Enterocele
An enterocele is a less common form of pelvic organ prolapse where the small intestine herniates down into the vaginal passage. Entrocele symptoms are more typical in the absence of a uterus, although it can happen with the uterus still in place (sometimes referred to as enterocele caused by apical prolapse). Enterocele symptoms are common with a vaginal vault prolapse following hysterectomy. Hysterectomy destabilises the supportive ligaments of the uterus which can contribute to formation of an enterocele. Pelvic organ prolapse is measured in stages ranging from stage 1 which is a minor prolapse, to stage 4 which is complete prolapse. Surgery is almost always required for this type of prolapse. If you believe you may have this type of pelvic organ prolapse, you should see a pelvic floor physical therapist (physiotherapist) or gynecologist.
Stage 4 Enterocele
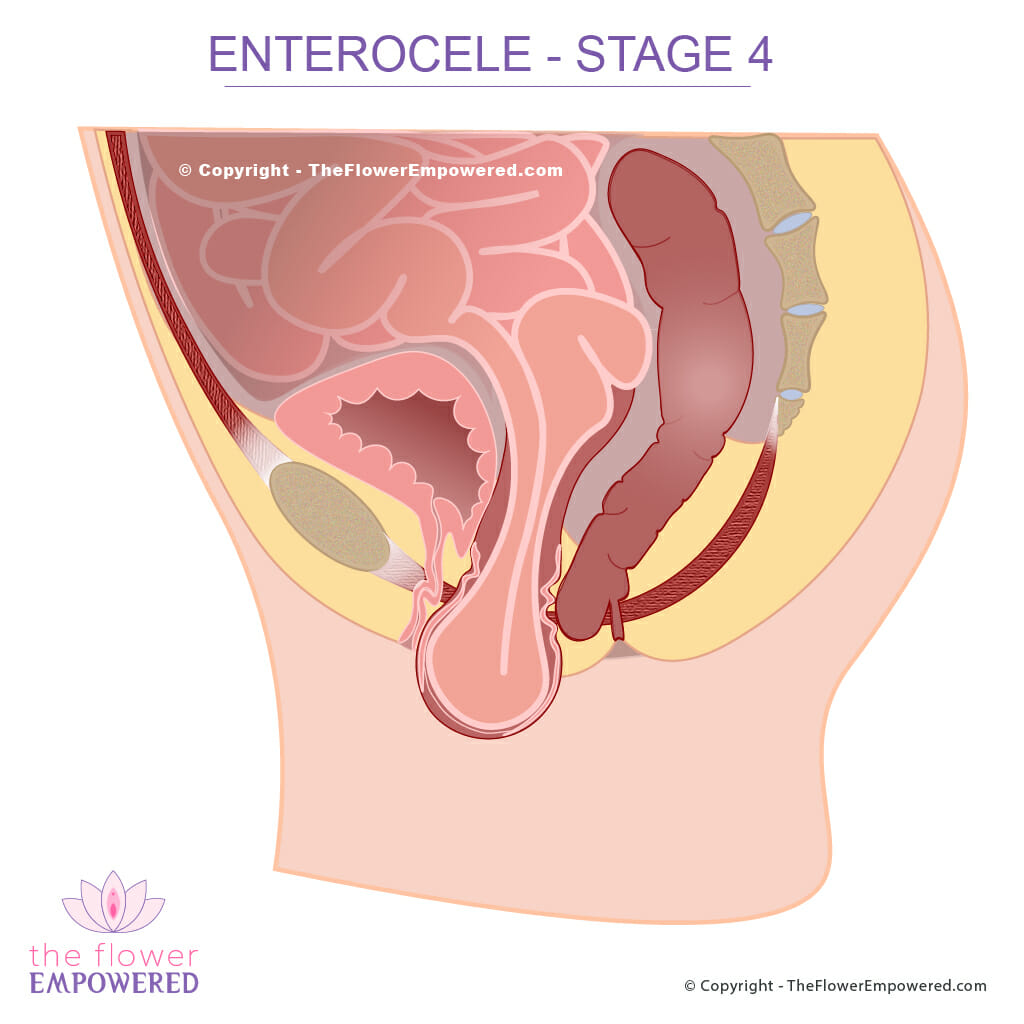
Considerations When You Have an Enterocele
Because the enterocele causes the small intestine to slip down into the vagina, digestion and bowel function can be impacted. Urine function can also be impacted, depending on the stage of this pelvic organ prolapse. An enterocele can also have negative impact on sexual function.
Treatment for Enterocele
Due to enterocele normally being caused by an earlier surgery to remove the uterus, a subsequent surgery is often required to repair the enterocele. Sometimes conservative treatments are also recommended to improve the overall function of the pelvic floor and support for the organs. Click on the relevant button below to find out more about conservative (non-surgical) and invasive (surgical) treatments for prolapse. If you did not find what you were looking for, you can search this site using the search bar at the bottom of the page.
Explore the Other Types of Pelvic Organ Prolapse
Having reviewed the enterocele, you may be interested in exploring the other types of prolapse. You can do that from here:
References
- Barber MD, Maher C. Epidemiology and outcome assessment of pelvic organ prolapse. Int Urogynecol J. 2013 Nov;24(11):1783-90. doi: 10.1007/s00192-013-2169-9. PMID: 24142054.
- Pelvic Organ Prolapse, Female Pelvic Medicine & Reconstructive Surgery: 7/8 2017 – Volume 23 – Issue 4 – p 218-227 doi: 10.1097/SPV.0000000000000430
- Aboseif C, Liu P. Pelvic Organ Prolapse. [Updated 2021 Oct 9]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK563229/
- Dischiavi SL, Wright AA, Hegedus EJ, Bleakley CM. Biotensegrity and myofascial chains: A global approach to an integrated kinetic chain. Med Hypotheses. 2018 Jan;110:90-96. doi: 10.1016/j.mehy.2017.11.008. Epub 2017 Nov 20. PMID: 29317079.