30% of women with incontinence will suffer mixed incontinence1
What Is Mixed Urinary Incontinence (MUI)?
Mixed urinary incontinence symptoms are a combination of stress incontinence (leakage during activity) and urge/frequency symptoms of overactive bladder. Oftentimes, mixed incontinence is a result of “Just incase” peeing (JIC). When you suffer from stress incontinence, you have a tendency to urinate before leaving the house and immediately on arriving to your destination. This is due to the fear of leakage. By JIC peeing, you negatively reprogram your bladder to think that it is full when in reality, it contains a small amount of urine. Over time, this leads to the symptoms of overactive bladder. You can read more about negative bladder programming on the OAB page. On this short page, we will focus on considerations specific to mixed incontinence.
With mixed urinary incontinence, the amount of leakage can vary greatly. Anything from a few drops to soaking through your clothing and down to the floor. Studies have shown the Sandvik test to be a good measure of the severity of your incontinence. We have created an online version of the Sandvik test to help you determine your level of incontinence. Minimum score 0, maximum score 12. A higher score indicates a higher degree of incontinence.
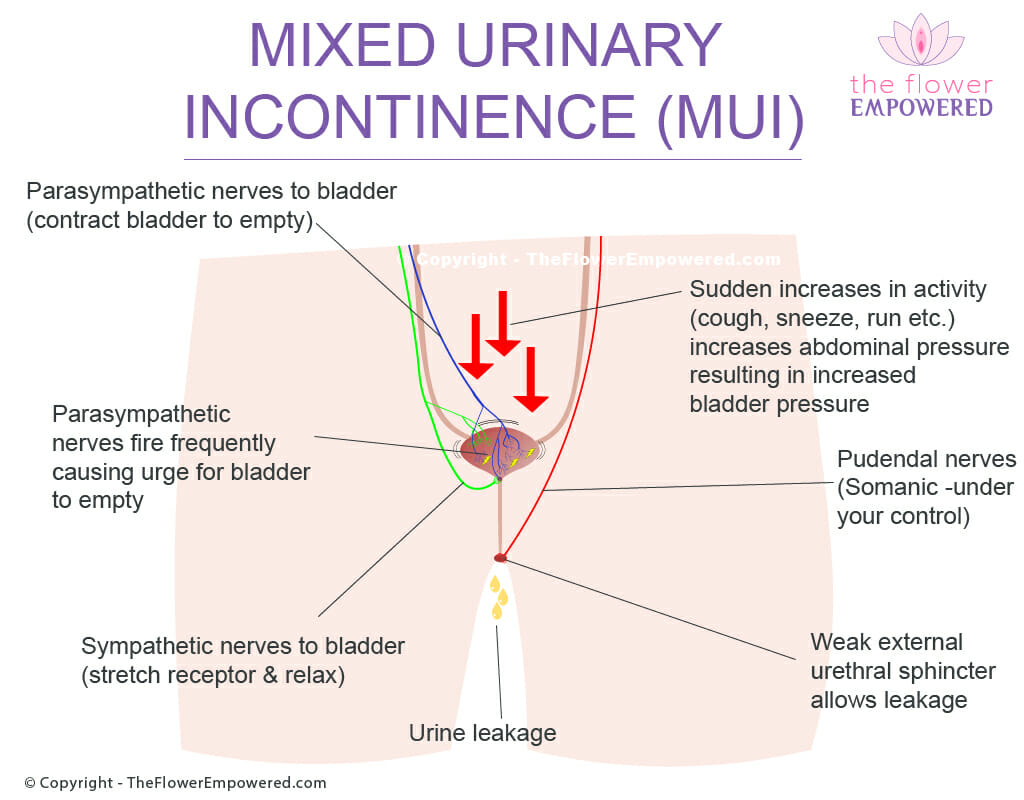
The small yellow electric shock’s on the image attempt to convey how the OAB symptoms with mixed incontinence trigger signals to empty. The red arrows attempt to convey an increase in intraabdominal pressure. Mixed incontinence can manifest in different ways for different people. If you find yourself experiencing the symptoms of mixed urinary incontinence, you should see your doctor.
When suffering from mixed urinary incontinence symptoms, your treatment will be similar to that of overactive bladder but with a strong emphasis on pelvic floor muscle training (PFMT). Studies show that women with weaker pelvic floor muscles show the greatest percentage improvement when undertaking PFMT.
Consistency is key, both with your bladder training and your pelvic floor muscle training (PFMT). Increasing the strength of your external urethral sphincter has the added benefit of enhancing the guarding reflex thus helping to reduce your symptoms of urgency. Your pelvic floor physiotherapist and urologist can help you to set goals that are achievable.
Treatment Options for Urinary Incontinence
Like most symptoms of pelvic floor dysfunction, the treatment for urinary incontinence falls into one of two categories; conservative (non-surgical) and invasive (surgical). Surgical options are generally only advised for once conservative options have been tried unsuccessfully for an extended period. For more information on the various treatments offered in these two categories, click on the relevant button below. If you did not find what you were looking for, you can search this site using the search bar at the bottom of the page.
Explore the Other Types of Urinary Incontinence
Having reviewed the Mixed Urinary Incontinence, you may be interested in exploring the other types of incontinence. You can do that from here:
References
- Tran LN, Puckett Y. Urinary Incontinence. [Updated 2021 Aug 11]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK559095/.